Battling Disease & Debt: Financing Non-Communicable Diseases Amidst Economic Crisis
By Sunimalee Madurawala:
Introduction
“The
shortage of medicines will significantly impact medications for non-communicable
diseases (NCDs). If NCD patients don’t receive their regular medication, their
condition will worsen,” stated a Provincial Director of Health Services
speaking on the implications of the economic crisis on NCDs. Over the last few
decades, NCDs have emerged as a critical health challenge for Sri Lanka,
placing a significant burden on the country’s healthcare system. More
than 80 % of the total deaths that occurred in the country are
due to NCDs. NCDs
accounted for 38% of the country’s total health expenditure in 2019,
amounting to USD 1,183 million. The economic impact is particularly challenging
for households
affected by chronic NCDs as they bear higher costs of
medicines, pharmaceutical products, medical laboratory tests, and other
ancillary services. With the current economic downturn, preventing and
financing NCDs has become even more challenging for Sri Lanka.
An ongoing IPS study delves into the
implications of the economic crisis on the country’s health system, with a specific
focus on NCD prevention and financing. The study conducted an extensive
analysis by gathering perspectives from various stakeholders. This blog is
based on the information collected from these stakeholders.
Economic
Crisis and Sri Lanka’s Health System
The COVID-19 pandemic has already put Sri Lanka’s health sector under
intense pressure, and
the ongoing economic crisis has added more stress to the sustainability of the
country’s healthcare system. An economic crisis can directly
and indirectly impact a health system. For
instance, during times of economic crisis, it’s common for governments to
reduce their social expenditures, and one area that could be affected is
healthcare. This could result in cuts to health budgets. Furthermore, the
demand for healthcare services will decrease, particularly in the private
sector, where treatment costs could increase. Additionally, child and maternal
nutrition and other health outcomes will deteriorate
as with the increasing food prices, people opt to reduce food quantity and
quality.
Once well-recognised for its strength and cost-effectiveness,
Sri Lanka’s health system is now challenged by knowledge, capacity, and policy gaps.
The economic crisis would undoubtedly worsen these gaps, even
to the point of the collapse of the health system. The adverse impacts of the economic crisis could hinder the laudable
progress achieved by the country over the years, leading to an
increase in NCDs, malnutrition among children, communicable diseases, and
mental health issues.
Implications
on NCDs
The
economic crisis in Sri Lanka has significant short-term and long-term
implications for NCD prevention and financing. In the short term, the shortage
of medical supplies has become the most pressing concern. Further, resource
limitations have resulted
in the delay or limitation of lab tests and surgeries, including non-essential and non-urgent
surgeries at government hospitals. In addition, the fuel shortage which escalated
last year has severely impacted preventive care services, curative care
services, and administrative functions at all levels of the health sector, weakening the
entire health delivery mechanism. Moreover, the government’s
decision to limit capital expenditure would have serious negative repercussions
on maintaining the existing NCD service delivery and catering to the increasing
demand for NCD preventive (e.g., awareness campaigns and screening programmes) and
curative (e.g., construction of hospitals and clinics) measures in the future.
Participating
in one of our interviews, an officer from a Provincial Health Ministry stated
that, in the long term,” the prevalence of risk factors will
undoubtedly increase eventually, and individuals who already suffer from NCDs
may find it challenging to manage their conditions.” For example, the
prevalence of unhealthy dietary patterns – one of the NCD behavioural risk
factors – is likely to become more prevalent. Even before the economic crisis, Sri
Lanka’s nutrition indicators stood at a lower level and there was limited
progress towards achieving the diet-related non-NCD targets. The
high food prices have compelled people to either reduce or avoid consuming
healthy foods or opt for cheap, unhealthy foods. This would “lead to a
decline in earning and learning capacities for the next generation resulting in
generational effects”, feared a Provincial Health Ministry officer.
Becoming More
Resilient and Facing the Challenges – the Way Forward
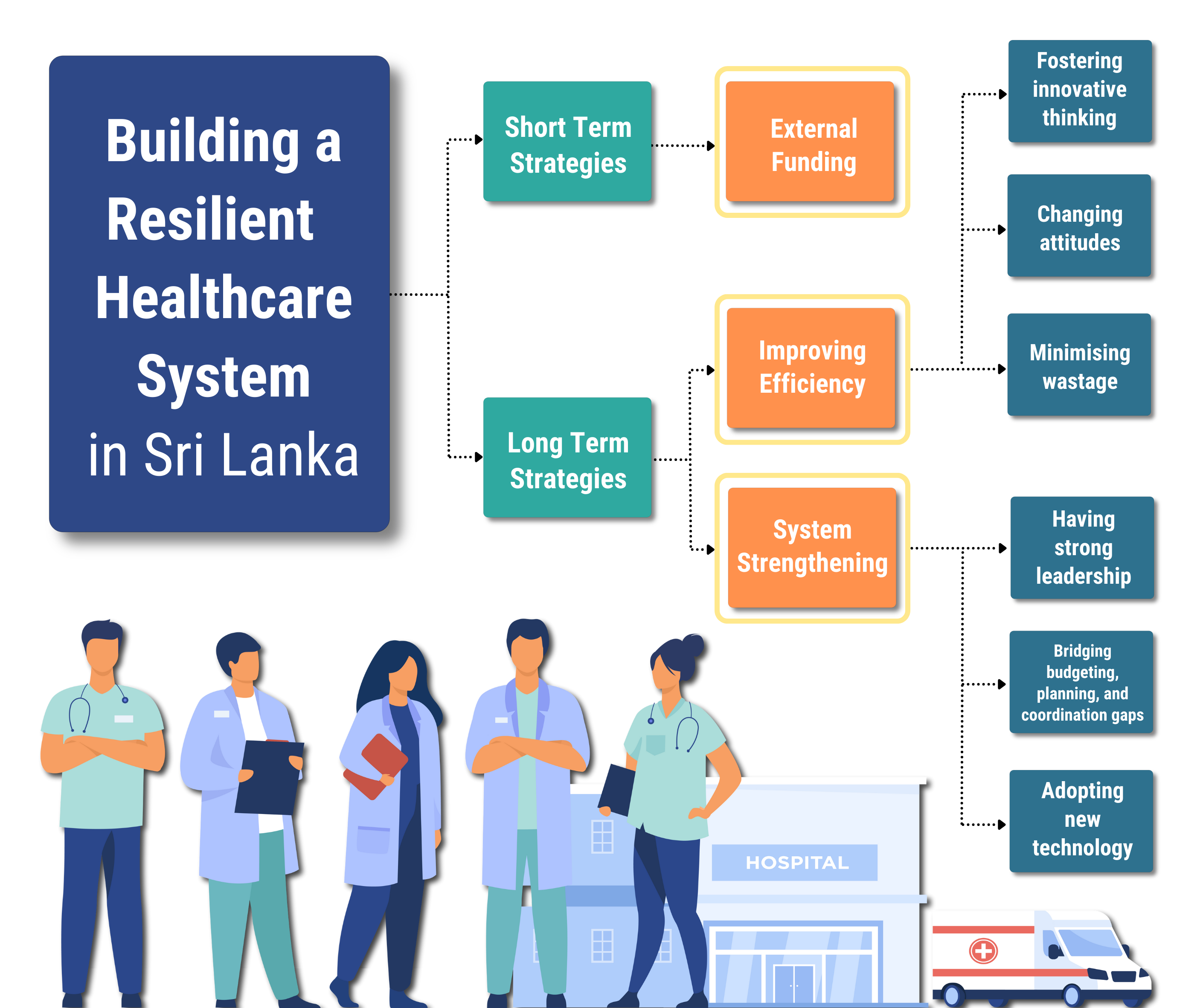
Most
stakeholders who participated in this study suggested that seeking external
funding is the most suitable short-term strategy for Sri Lanka to finance NCDs
to overcome the current crisis. “We (the country) should also aim to receive
more foreign aid instead of loans, which requires close discussions with other
countries and international organisations suggested a senior officer from
the Ministry of Health.
While
seeking external support as a short-term relief, it is crucial to focus on
long-term strategies to improve the resilience of Sri Lanka’s healthcare system
in handling future crises.
Improving
efficiency and strengthening the system are vital long-term strategies proposed
by the stakeholders in building a more resilient healthcare system.
Minimising
wastage, changing attitudes, and fostering innovative thinking should be the
key pillars of increasing efficiency, as indicated by the stakeholders. Likewise,
system strengthening requires strong leadership, the use of technology, and
paying more attention to budgeting, planning, and coordination. Additionally, exploring
alternative financing ventures, restructuring the health financing system, and
focusing on smarter
spending are necessary as providing citizens with free
healthcare becomes increasingly challenging for the government in a limited
fiscal space. Such measures would make the country’s healthcare system robust
which can withstand both the short-term and long-term consequences of a crisis,
assured the stakeholders who participated in this study.
Despite
the severe impact of the current economic crisis on NCD prevention and
financing efforts, it provides an opportunity to understand the gaps in the existing
system and develop a more sustainable and resilient healthcare system to cater
to the increasing demand for NCD prevention and financing.
* This
study is carried out in collaboration with the Center for Policy Impact in
Global Health (CPIGH) of Duke University with financial support from the Bill
and Melinda Gates Foundation.
Sunimalee Madurawala is a Research Economist at IPS. Her research interests include health economics, gender and population studies. Sunimalee holds a BA (Economics Special) with First Class Honours and a Masters in Economics (MEcon) from the University of Colombo, Sri Lanka. (Talk to Sunimalee – sunimalee@ips.lk)